Supporting newly qualified diabetes nurses achieve credentialling and experience across tertiary, secondary and primary diabetes care settings: Diabetes Tasmania’s Internship Program.

Introduction
Worldwide the prevalence of diabetes has risen from 4.7% in 1980 to 8.5% in 2014. 1 The number of adults with diabetes increased from 108 million in 1980 to 422 million in 2014 and is predicted to surpass 700 million by 2025, if current trends continue. 2 Australia has seen a similar trend with a tripling of diabetes prevalence from 1989-90 to 2017-18 (1.5% to 4.9% respectively) and just over 1.3 million people registered with diabetes on the National Diabetes Services Scheme (NDSS). 3, 4
Diabetes care is under pressure, not simply due to the sheer increase in prevalence, but the exponential increase in the complexity of care that comes with being older and more disadvantaged by remoteness, socioeconomic or Indigenous status. 5, 6
A diabetes educator relies not only on specialist knowledge and technical expertise, but also their experience in delivering education to individuals and groups with various levels of education, health literacy cultural and economic backgrounds. 7 In Australia, this experiential knowledge is difficult to attain for entry level diabetes educators due to a paucity of positions and the high number of qualified applicants. Much of the technical expertise, such as insulin pumps and continuous glucose monitoring device management, is not covered beyond theory in the postgraduate coursework. This places newly qualified diabetes educators in the ironic situation of requiring skills for a job that they can only attain if they have the job. Workplaces are also under pressure to provide training and upskilling of new graduates in the setting of ever-increasing demands on resources and time. In this context, Diabetes Tasmania developed the David Symons Memorial Scholarship in 2016 to support a newly qualified diabetes educator (DE) enter the specialist diabetes workforce.
Diabetes Educators in Australia
The Australian Diabetes Educator Association (ADEA) defines a diabetes educator as a health professional who delivers diabetes education, self-management support and motivation to people living with diabetes.8 This definition does not take into consideration education, experience or scope of practice. The challenge in identifying a diabetes educator is that the role is broad, not clearly defined and can be undertaken by a number of health care professionals (registered nurses, exercise physiologists, dietitians, pharmacists, midwives, medical practitioners and physiotherapists) in different health care sectors.7 This is further complicated by the fact that a diabetes educator can practice without being credentialled by the ADEA as there is currently no mandatory requirement to be credentialled.
The ADEA is the peak professional body for diabetes educators that among other things, accredits postgraduate courses across the country, provides standards and guidelines for practice, and oversees the Credentialling and Re-credentialling Program which it established to formally maintain minimum professional standards of practice and care in diabetes management.9 In 2017, the ADEA released a document outlining the National Competencies for Credentialled Diabetes Educators which distinguished beginner, experienced and expert scope of practice.10 This is an important consideration in ensuring quality diabetes education services are delivered by experienced healthcare professionals working within their scope of practice. This is comparable to standards held by international diabetes educator colleges and associations (see Figure 1).
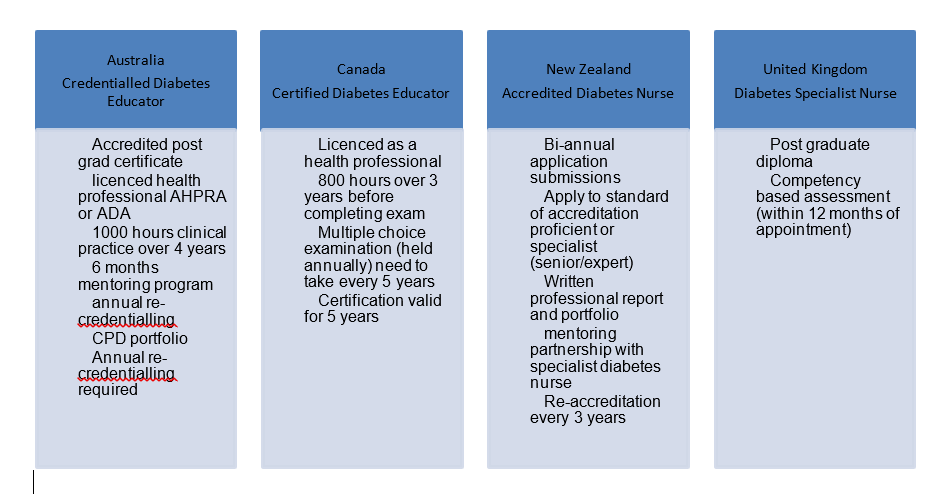
Figure 1. Requirements for initial credentialling in Australia, Canada, New Zealand and the United Kingdom. 9, 11, 12, 13
In 2017, there were 1,308 Credentialled Diabetes Educators (CDE) in Australia, 78% of who were registered nurses (RNs).14 What is not known is the number of RNs working as diabetes educators without being credentialled. The ratio of diabetes registrants (1.3 million) to CDEs being what it is, there is necessarily a large number of practice nurses working within the role of diabetes educator without postgraduate education and little specialist experience.6, 15
One of the challenges for those who have completed their postgraduate diabetes course is to gain the hours of work in the field to become credentialled. This can be difficult if they are not already employed as a diabetes educator. Regardless of where the hours were obtained, there is no current process of assessing the quality of the education delivered. For example, nurses who have completed the certificate could count the hours working in aged care or as a practice nurse completing care plans towards their 1000 hours. This raises the issue around how effective these hours are in supporting experience and skill acquisition in working towards becoming a CDE.
A 2016 ADEA survey of diabetes educators identified that that 6% of 595 respondents, were not employed in diabetes care but actively seeking such work.16 This number is likely to be an underestimation. With at least five institutions offering the accredited postgraduate certificate in diabetes management and an estimated 500 health professionals completing it each year, the question of how to overcome the bottleneck of transition into practice as a CDE is an important one. Of course, there are broader questions with the nature of the workforce in diabetes, given the epidemiology and changing technologies and medications affecting delivery of appropriate care in the future. Nevertheless, the scholarship initiative undertaken by Diabetes Tasmania, offers a template for other organisations to consider.
The Diabetes Tasmania Internship Program
While there is a higher ratio of CDEs per diabetes registrants in Tasmania compared to New South Wales (NSW), for example (1 CDE/700 in Tasmania, 1 CDE/2200 in NSW),14 Diabetes Tasmania recognised a need to continue to attract new diabetes educators to the state and provide them with an opportunity to train across a number of health care settings. In 2016 Diabetes Tasmania funded the inaugural 12 month position for a newly qualified DE to work in a training role while meeting the criteria for credentialling status. The scholarship was named after David Symons who, with his wife Janet, was a long-term donor and supporter of the organisation.
The scholarship funded 0.6FTE and involved rotation between three clinical sites: Diabetes Tasmania, general practice and a tertiary hospital diabetes centre. This ensured clinic experience in diabetes across numerous settings: from high risk foot clinic, gestational diabetes clinics, inpatient care, as well as paediatrics and training in insulin pumps and continuous glucose monitoring. The recipient also worked within a suburban GP clinic one day a week, and had opportunities to attend rural clinics, type 1 youth camps, and deliver group education to nurses and allied health staff in aged care, hospital and community care. The scholarship also supported the recipient through the ADEA credentialling program.
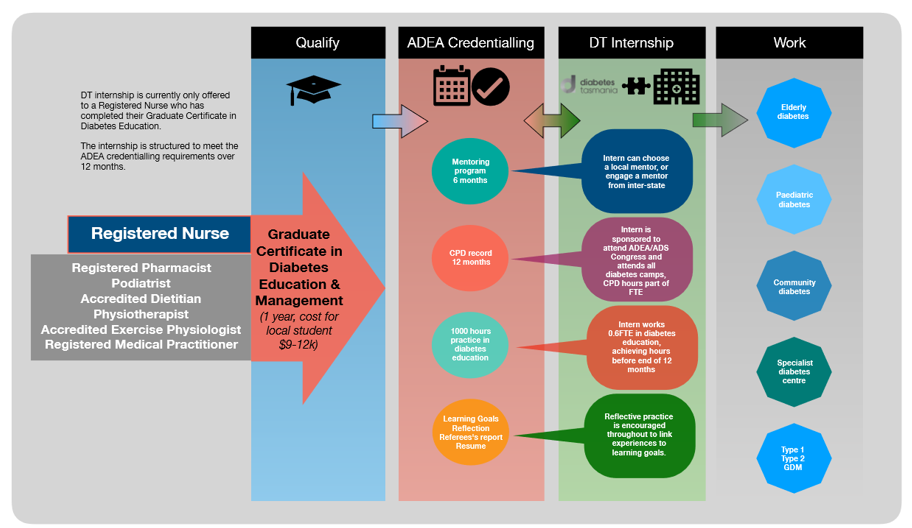
Figure 2. Implementation and plan of activities during internship with Diabetes Tasmania
Two recipients have undertaken the scholarship successfully and achieved and maintained credentialling. After the first two years, the scholarship program was postponed for a year to allow review of the experiences and approach for future recipients. Changes to the ADEA credentialling program were also taken into consideration. The first change was to re-classify the program as an internship, reflecting the expectations of a beginner level DE progressing over the next 12 months, as per the ADEA level of practice criteria. The second change included development of a Recipient Handbook outlining the aims, professional learning outcomes, details of the credentialling process and a schedule of activities. This includes quarterly aims and learning outcomes linked both to personal learning and learning goals required for credentialling. A Clinical Practice Worksheet was developed as a template for the intern to log their activity hours, learning needs and outcomes and receive feedback from supervisors or preceptors. The intern would receive structured exposure to clinical practice from observing, to supervised and eventually independent levels in the range of clinics and settings.
Unfortunately, the last recipient needed to return interstate for personal reasons. Consequently, the position will be advertised later in 2019 with the expectation that a successful applicant will commence the internship in 2020. The first two recipients are now working as CDEs in Hobart in paediatric diabetes, rural clinics and on a number of projects including aged care. The experience has given them a broad range of clinical skills and knowledge which has allowed them to engage dynamically with different age groups and backgrounds and across the various sectors of healthcare.
This initiative has demonstrated the benefits of a structured support pathway from theory to practice for RNs who wish to become CDEs. There may be scope for future internships to be offered to other health professionals, however it is currently only offered to RNs. While it is limited in providing access to one nurse per year, its strength is in training highly specialised CDEs with the diversity of diabetes care experience and skills much needed in tackling the growing complexity and prevalence of diabetes in Australia. It serves as a blueprint for similar programs that could potentially be implemented in a number of healthcare settings, not only through other diabetes organisations, but within specialist primary and secondary care settings across the country.
One of the key strengths of the program has been the collaboration between the tertiary diabetes centre and the community sector demonstrating the importance of partnerships in these types of initiatives. What we have learned from two years of this program is the value in developing specialist diabetes educators whose practice is not only benchmarked by standards and underpinned by evidence-based practice, but incorporates clinical and peer review and support from mentors and experienced CDEs within the ADEA’s credentialling program remit.
Conclusion
The continuing rise of diabetes prevalence in Australia, especially when one considers the highest risk populations, raises questions of the sustainability of the future workforce in diabetes care. There is an international agreement that diabetes care and prevention requires a multidisciplinary approach that supports people not only at diagnosis, but across the life span, with appropriate self-management education. Central to this approach is the role and availability of diabetes educators. In Australia, there is a need to assist newly qualified diabetes educators achieve ADEA credentialling status while developing their clinical skills from beginner to independent in a structured, peer-reviewed way. The Diabetes Tasmania internship program is an example of how this can be done.
If you are interested in applying for the 2020 internship or would like further information about the program, please contact Diabetes Tasmania mail@diabetestas.org.au
References
1.World Health Organization. Global Report on Diabetes [Internet]. City: France; 2016 [cited 2019 Feb 26]. p. 25. Available from https://apps.who.int/iris/bitstream/handle/10665/204871/9789241565257_eng.pdf;jsessionid=0C082BB7DB19E7331B06BBF2FAACDF18?sequence=1
2.NCD Risk Factor Collaboration (NCD-RisC. Worldwide trends in diabetes since 1980: a pooled analysis of 751 population-based studies with 4.4 million participants. The Lancet. 2016 Apr [cited 2019 May 8]. 387:1513-30. Available from DOI https://doi.org/10.1016/S0140-6736(16)00618-8
3.National Diabetes Services Scheme. Diabetes Map [Internet]. City: Canberra AU: Diabetes Australia 2019 [cited 2019 Feb 26]. Available from https://map.ndss.com.au/#!/
4.Australian Bureau of Statistics. National Health Survey: First Results, 2017-18 [Internet]. City: Canberra AU 2018 [cited 2019 Nov 11]. Available from https://www.abs.gov.au/ausstats/abs@.nsf/Lookup/by%20Subject/4364.0.55.001~2017-18~Main%20Features~Diabetes%20mellitus~50
5.Sinclair, A. J., Abdelhafiz, A. H., Forbes, A. and Munshi, M. Evidence-based diabetes care for older people with type 2 diabetes: a critical review. Diabetic Medicine. 2019. 36(4):399-413.
6.Australian Institute of Health and Welfare. Diabetes snapshot. City: Canberra AU. 2018 [cited 2019 Jun 21]. Available from https://www.aihw.gov.au/reports/diabetes/diabetes-snapshot/contents/how-many-australians-have-diabetes
7.Burke S. Sherr D. Lipman R. Partnering with diabetes educators to improve patient outcomes. Diabetes, Metabolic Syndrome and Obesity: Targets and Therapy. 2014 [cited 2019 May 8]; 7:45-53. Available from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3926770/
8.Australian Diabetes Educators Association. Role and Scope of Practice for Credentialled Diabetes Educators in Australia. 2015 [cited 2018 Feb 7]. Available from https://www.adea.com.au/wp-content/uploads/2009/10/Role-and-Scope-of-Practice-for-Credentialled-Diabetes-Educators-in-Australia-Final1.pdf
9.Australian Diabetes Educators Association. Quick Guide to Initial Credentialling [Internet]. 2015 Oct [cited 2018 Jan 10]. Available from https://www.adea.com.au/wp-content/uploads/2014/10/A-quick-guide-to-preparing-your-application-for-Initial-Credentialling-1.pdf
10.Australian Diabetes Educator Association. National Competencies for Credentialled Diabetes Educators [Internet]. City: Canberra AU. [cited 2018 Feb 21]. Available from https://www.adea.com.au/wp-content/uploads/2009/10/National-Competencies-for-Credentialled-Diabetes-Educators_Final_170824-1.pdf
11.The Canadian Diabetes Educators Certification Board. How to become a certified diabetes educator [Internet]. 2018 [cited 2018 Jan 10]. Available from http://www.cdecb.ca/what-is-a-cde/how-to-become-a-cde/
12.Aoteaora College of Diabetes Nurses. Accreditation [Internet]. 2014, updated 2018 [cited 2018 Jan 10]. Available from https://www.nzno.org.nz/groups/colleges_sections/colleges/aotearoa_college_of_diabetes_nurses/accreditation
13.Diabetes United Kingdom (UK). Diabetes Specialist Nurses [Internet]. 2019 Mar [cited 2019 Sep 11]. Available from https://www.diabetes.org.uk/resources-s3/2019-03/Position%20statement%20defining%20who%20is%20an%20Adult%20Diabetes%20Specialist%20Nurse.pdf?
14.Freeman R. Membership Data 2017 [online] email to M Clarkson Fletcher (mclarksonfletcher@diabetestas.org.au) 2017 Jun 15 [cited 2017 Jun 15]
15.Hollis M. Glaister K. Lapsley JA. Do Practice Nurses Have the Knowledge to Provide Diabetes Self Management Education? Contemp Nurse [Internet]. 2014 [cited 2018 Feb 21]; 46(2):234-41. Available from DOI 10.5172/conu.2014.46.2.234
16.Australian Diabetes Educator Association. Workforce in Diabetes Education [Internet]. Date Unknown [cited 2018 Feb 19]. Available from https://www.adea.com.au/resources-2/workforce-in-diabetes-education